How can you remove a tick – and what’s the best way to avoid ticks in the first place?
How to remove a tick
If you find a tick attached to your skin, there’s no need to panic. There are several tick removal devices on the market, but a plain set of fine-tipped tweezers will remove a tick quite effectively.
DO NOT use petroleum jelly, a hot match, nail polish, or other products to make the tick detach from the skin. Your goal is to remove the tick as quickly as possible — not waiting for it to detach.
How to remove a tick
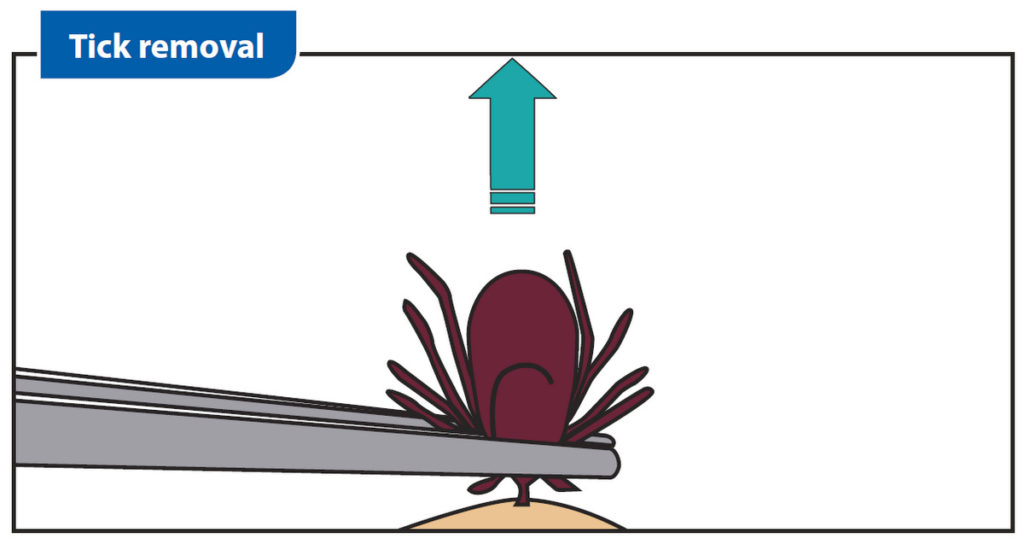
- Use fine-tipped tweezers to grasp the tick as close to the skin’s surface as possible.
- Pull upward with steady, even pressure. Avoid crushing the tick’s body. Don’t twist or jerk the tick; this can cause the mouth-parts to break off and remain in the skin. If this happens, remove the mouth-parts with tweezers. If you are unable to remove the mouth easily with clean tweezers, leave it alone and let the skin heal.
- After removing the tick, thoroughly clean the bite area and your hands with rubbing alcohol, an iodine scrub, or soap and water.
Follow-up
If you develop a rash or fever within several weeks of removing a tick, see your doctor. Be sure to tell the doctor about your recent tick bite, when the bite occurred, and where you most likely acquired the tick.
How to avoid tick bites
Before you lace up your hiking boots and head to the great outdoors, take note.
Every year, thousands of adults, children and pets across the country are exposed to Lyme disease and other diseases carried by ticks. Simple precautions can help you avoid getting sick from these blood-feeding creatures.
In 1975, 51 people came down with a mysterious arthritis-like ailment in Lyme, Connecticut. NIH researchers discovered that the disease was caused by small, coiled bacteria called Borrelia burgdorferi, or simply Bb. The bacteria spread to humans from the bite of a tiny deer tick. The tick can be as small as a pinhead.

Lyme disease is now the most common tick-borne disease in the United States. The incidence of Lyme disease in the United States has approximately doubled since 1991, from 3.74 reported cases per 100,000 people to 7.95 reported cases per 100,000 people in 2014.
As of 2018, it was noted that each year, approximately 30,000 cases of Lyme disease are reported to CDC by state health departments and the District of Columbia. However, this number does not reflect every case of Lyme disease that is diagnosed in the United States every year.
Most were in the Northeast and Midwest, but people in all 50 states are at risk. Ticks can also transmit other diseases, including Rocky Mountain spotted fever, ehrlichiosis and anaplasmosis. Peak tick season is in June, July and August.
A deer tick can live on a variety of warm-blooded animals. Immature ticks favor small mammals, while adults tend to feed on white-tailed deer. The small mammals that ticks feed on can act as reservoirs for Bb, harboring it in their bloodstream.
After a tick takes a blood meal from an infected animal, or host, the bacteria remain in the tick’s gut throughout its life. The tick can then infect any new creature it feeds upon, including humans. However, transmission of Bb to a new host requires 24 to 48 hours.

That’s why it’s important to carefully check your body and clothing for ticks after being outdoors in woody and grassy areas. If you see a tick, you can lessen the chance of infection by removing it from your body early, even if it’s already begun to feed.
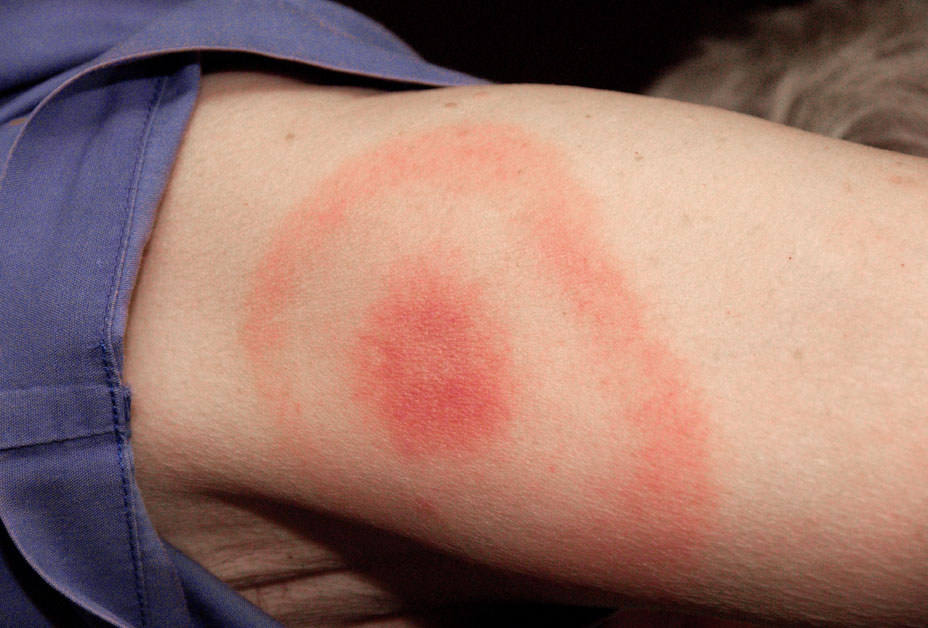
A bull’s-eye shaped rash at the site of the tick bite is the most reliable early symptom of Lyme disease. It appears 3 to 32 days after a tick bite in 70-80% of cases. The rash has a dark spot in the center where the bite was, with a lighter color ring around the spot.
Other early symptoms of Lyme disease resemble those of the flu. Warning signs include fatigue, headache, joint stiffness, stiff or painful muscles, fever and swollen joints.
If the disease progresses, symptoms such as irregular heartbeat, heart palpitations or neurological abnormalities can develop. In its most advanced stages, Lyme disease can be debilitating.
“Early treatment is the most effective way to clear the infection from the body,” says Dr Joseph Breen of NIH’s National Institute of Allergy and Infectious Diseases. The key is to consult a health care provider as soon as you recognize any symptoms.
“Scientists are currently working to understand how Bb interacts with its host,” says Breen. “In addition, work is underway to develop more effective diagnostic tools and vaccines.”
Gardening, camping, hiking and just playing outdoors are all great spring and summertime activities. But make tick prevention a part of your routine.
What you can do to protect yourself
You can decrease the chances of being bitten by a tick with a few precautions.
Avoid tick-infested areas. This is especially important in May, June, and July. Many local health departments and park or extension services have information on the local distribution of ticks. If you are in tick-infested areas, walk in the center of trails to avoid contact with overgrown grass, brush, and leaf litter at trail edges.
Use insect repellent. Spray repellent containing a 20% concentration of DEET on clothes and on exposed skin. You can also treat clothes (especially pants, socks, and shoes) with permethrin, which kills ticks on contact, or buy clothes that are pre-treated. Permethrin can also be used on tents and some camping gear. Do not use permethrin directly on skin. Always follow the manufacturer’s instructions when applying any repellent.
Perform daily tick checks. Always check for ticks after being outdoors, even in your own yard. Because ticks must usually be attached for at least a day before they can transmit the bacteria that cause Lyme disease, early removal can reduce the risk of infection.
Bathe or shower. Bathe or shower as soon as possible after coming indoors (preferably within 2 hours) to wash off and more easily find ticks that are crawling on you. Ticks can get a ride indoors on your clothes. After being outdoors, wash and dry clothing at a high temperature to kill any ticks that may remain on clothing.